
One of our main priorities is to ensure universal access to, and informed use of effective contraception. Millions of people lack the knowledge and information to determine when or whether they have children, and they are unable to protect themselves against sexually transmitted infections (STIs).
Articles about Contraception

“I wanted to work with the parents so we can stop marrying off these girls too young”
Komi Agnimavo Amazoun becomes visibly angry when he recalls the phone call telling him a 16-year-old girl was to be married off from his village in central Togo. As the highly respected village chief of Detokpo, a community of a few hundred people, Amazoun had the final say on the union, which later turned out to be the result of an attempted cover-up of a rape. Forced early marriage “I saw that she was being married off too young. The parents came to see me and I said she was not the right age,” the usually softly spoken elder said. “She didn’t yet have an education or a job” and says the girl is now 18 and has started an apprenticeship in tailoring. Such successful interventions by village chiefs in ending forced early marriage reflects the crucial importance of their involvement in sexual health strategies in the country especially in rural areas. Detakpo is one of 870 villages which have signed Village Girl Protection Charters to stop forced transactional sex in rural communities, in an initiative promoted by the Association Togolaise Pour le Bien-Être Familial (ATBEF). The charters outline prevention measures and rules in line with Togolese law to stop the rape and exploitation of underage girls, who are particularly vulnerable outside urban areas where professional advice and protection are more easily reached. Working with parents Amazoun has also received training from ATBEF on the law, which bans marriage under 18 without parental consent, and on the use of contraception to prevent underage pregnancy. “We have started to raise awareness in the village so that similar cases won’t be repeated,” Amazoun said, sitting on a plastic chair outside his home. “I wanted to work with the parents so we can stop marrying off these girls too young,” he adds. Although the official rate of marriage under 18 in Togo stands at 22%, according to UNICEF, the true rate is likely much higher, as many weddings are village ceremonies that are never registered with the authorities. “This is a very traditional place with entrenched customs. The problem of sexual violence runs very deep, which means that we have cases upon cases to deal with,” explained Dopo Kakadji, the Director for Social Action in Haho Prefecture. Kakadji oversees sexual violence cases and child protection in the area, mediating disputes over marriage and providing a link between communities and the police when necessary. The future is looking promising In many households, he said, “the woman cannot make decisions for herself. She is an object that can be used as one likes. A father can exchange a daughter to resolve problems or for money”. However, his interventions, and the creation of youth clubs to inform children of their rights, has seen families increasing willing to denounce rapists publicly. “Today girls go to school. Things have changed in the last five years, because before the priority was to marry off daughters as soon as possible,” Kakadji noted. Photography by Xaume Olleros for IPPF
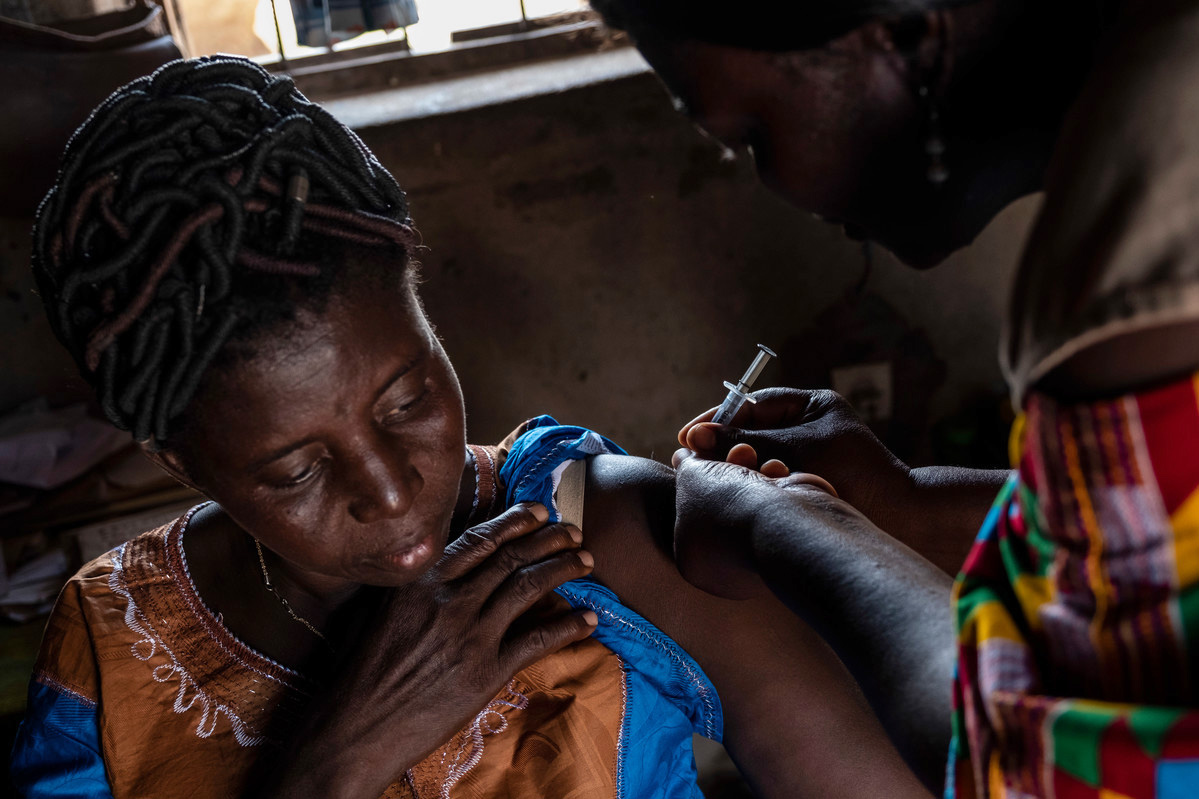
Togo: A country where contraception use is on the rise
Seated in an open-air classroom in the Togolese village of Tohoun, Adjo listens intently as her teacher leads a discussion about sexual harassment. At 13, Adjo is already aware of the dangers of teenage pregnancy and early marriage in her community and is learning how to handle boys trying to get her attention. “The boys really like chasing the girls and if you don’t know about that then you can get pregnant,” she said. “I want to finish my studies and have a boyfriend later.” Adjo is one of 410,000 young people who receive comprehensive sexuality education in schools and youth clubs in Togo, a country making huge strides in sexual healthcare provision. Youth & sex education Targeting youth in schools like Adjo’s is also a key focus. Young people have access to dedicated services at clinics in the country’s four regions, as well as outreach programmes for education and sexual healthcare, including HIV and STI testing in villages. “Last year there were about 15 girls pregnant, but since the ATBEF youth club started that has gone down a lot,” says 13-year-old Adjo. In Togo, 17% of young women will give birth before the age of 18. Through the Association Togolaise de Bien-Etre Familial (ATBEF), Togo now promotes the use of village charters to encourage the protection of girls from unintended pregnancy and gender-based violence. The decision of 870 villages to sign up to protection charters aimed at protecting girls and encouraging them to finish school has had a real impact. Men are taking an active role in the protection of women and young girls, and the delaying of pregnancy, through ATBEF’s village chief programme. “There have been problems with early pregnancy, but ATBEF encourages us to talk with young people, and to encourage them to use condoms,” explained Komi Agnimavo Amazoun, village chief of Detokpo, in central Togo. He intervened to stop a girl being forced to marry her rapist, a previously common practice in the area. “We have started to raise awareness in the village so that similar cases won’t be repeated,” Amazoun added. A rise in contraception use Togo, a nation of 7 million, has a fertility rate of 4.7 children per woman, according to the United Nations Statistics Division, but is aiming to cut it further. Since 2013, ATBEF more than 800 community health workers have been trained to advise and administer contraception nationally. ATBEF uses mobile clinics to reach rural areas and runs a successful clinic offering local men the option of non-surgical vasectomy - a rarity in the region. Based in the communities where they work, the health workers go door-to-door explaining the benefits of different contraceptive methods in local languages, building long-term trust. In the coming months, women will be able to administer contraceptive injections themselves in these communities, thanks to the introduction of the Sayana Press method. The prevalence of contraceptive use was at 17% before the community health worker programme began, a figure which has risen to 23% nationwide, according to government figures. “It’s no longer a taboo subject as it was in the 1980s, 1990s or 2000s,” explained Félicité Sonhaye, ATBEF Regional Coordinator for the central Plateaux region. “Today all women know about contraception, even if they don’t use it.” An increase in vasectomies Men in Togo are also increasingly considering long-term solutions to limit the number of children they support, especially while the country suffers an economic downturn. ATBEF is the only organization offering vasectomies in Togo and to date, 159 men have undergone keyhole vasectomy, despite strong cultural taboos surrounding men’s virility. “We thought men would not accept it but we quickly realized that there was an unmet need,” noted Sylvain Bingo M’Bortche, Chief of ATBEF’s Medical Division. “We have potential clients coming in and out [of Togo]. Men even come here from other countries, such as Benin, to benefit from vasectomies,” he added. Photography by Xaume Olleros for IPPF

"I’m so happy I now don’t have to worry about contraception for another five years”
In August 2017, weeks of continued and heavy rainfall across Nepal resulted in flash floods and landslides that affected 36 of the 75 districts. Many people lost their homes or were displaced. It was estimated that of those affected, 112,500 were women of reproductive age, including 8,694 pregnant women. IPPF Humanitarian, through their Member Association, The Family Planning Association of Nepal (FPAN), activated its emergency response system early on. With funding support from the Australian Government, FPAN and IPPF Humanitarian initially mobilised their response in four of the worst affected districts (Sunsari, Saptari, Bardiya, and Dang). Mobile medical camps were established to meet the sexual and reproductive health needs of the affected population, including through the distribution of short and long acting methods of contraception, STI and HIV screening, and GBV referrals. In collaboration with the USAID-SIFPO project, services were then expanded into five more affected districts. IPPF Humanitarian spoke with 21-year old Muna in her home district of Sunsari in Nepal. “I got married at 16 years old and have two children, a four-year-old girl and two-year-old boy. In my caste, we get married early, so my parents took me to get an arranged marriage. I was in the 8th class at the time, and returned to school after I got married, but only lasted one year. My husband works in construction and had to stop working for two weeks when the floods came. When he doesn’t work, he doesn’t get paid, so it’s been very difficult. A FPAN social worker told me about the mobile medical camp today. I used to be on the three-month injectable but today I changed to the five-year implant in my arm. When my youngest child was eight months old I found out I was pregnant again. I decided to discontinue that pregnancy, so I took the five small tablets given to me by my neighbourhood doctor. I was two months pregnant at the time. From this, I had two days bleeding and cramp like pain, and then weakness. I decided to abort that pregnancy because my youngest will still only eight months old, and I didn’t want any more children. If I had more than two children, it would be very difficult to feed and educate them, and would badly affect my body too. I’m so happy I now don’t have to worry about contraception for another five years.” Want to know more about safe abortion access? Join IPPF'S I Decide movement

What is pre-ejaculatory fluid (also known as pre-cum), and can it cause pregnancy?
There’s a good chance that you’re reading this because you are unsure of what pre-ejaculate (also known as pre-cum) fluid is, and if it can cause pregnancy. If you regularly use withdrawal as a contraception method, pre-ejaculate fluid is something you may want to know more about, especially if you are not planning a pregnancy or are worried about HIV and STIs. Read a quick round-up on the important things you should know about pre-ejaculate fluid. You can also watch our short animation on the effectiveness of the withdrawal (or ‘pulling out’) method. Pre-ejaculate is a natural lubricant Pre-ejaculate is a fluid that is discharged from a penis when it’s aroused and usually occurs right before ejaculation. The fluid acts as a natural lubricant during sex. It contains sperm Even though pre-ejaculate fluid comes from the ‘Cowpers gland’ (and not from testes like semen), some fluid can contain live sperm. A number of researchers believe this is a ‘cross-contamination’ from semen that may be present in the urethra from a previous sexual encounter, as both the pre-ejaculate fluid and semen pass through the urethra. It can cause pregnancy Although the chances of pregnancy from pre-ejaculate fluid is relatively low and can vary from person to person, 27% of those who use withdrawal as a regular form of contraception end up with a pregnancy. It can transmit STIs, including HIV Pre-ejaculate fluid can carry bacteria and viruses. Using the withdrawal method will not protect you from STIs, including HIV. If you are unsure of your partners’ status, consider another form of contraception. Men cannot control when it happens Most men cannot tell when they have pre-ejaculated. Withdrawal takes a lot of self-control, and in the heat of the moment, that can be a little difficult! So if you want to reduce the risk of STIs and HIV, and you’re not planning a pregnancy, you may want to use alternative contraception methods like the external condom or an IUD. To find out more about alternative contraception methods available to you visit our online guide to find the right option for you.

New flagship health programme to transform the lives of millions of women and girls
The lives of millions of women and girls will be transformed by new sexual and reproductive healthcare programmes led by International Planned Parenthood Federation (IPPF) and Marie Stopes International (MSI) consortia across Africa and South Asia. The programmes will launch integrated healthcare expansion in 27 countries and were announced in Kigali at the International Conference on Family Planning today. The Women’s Integrated Sexual Health (WISH) programme is funded by the UK Department for International Development (DFID), to deliver access to life-saving contraception for six million couples per year. The Secretary of State for International Development, Penny Mordaunt said: "Investing in family planning gives women control over their own bodies and lives. It helps them complete their education, pursue job opportunities and challenge inequality around the world." The new programme will accelerate progress towards meeting global commitments on expanding access to contraception made by governments and civil society organisations through the Family Planning 2020 (FP2020) movement. The IPPF and MSI WISH consortia will ensure previously unreached people, especially young and poorer women, are able to access contraception and have the choice on whether, when and how often to have children. IPPF’s Director General Dr Alvaro Bermejo said the WISH programme would transform lives. He said: "This is a significant investment and a deep commitment to putting women at the heart of healthcare. Women and girls – of all ages, places, income and education – must have access to high quality, voluntary family planning care and information. We thank the UK Government for their commitment to this vital issue. Together, we can accelerate change by expanding integrated healthcare through our clinics and outreach services. More services, wider contraceptive options and better access to safe abortion, means the right care at the right time. More power for every girl and woman to decide what to do with her body, with her life, and with her future." The WISH programme will scale up efforts at country level, expanding reach to millions of new users of sexual and reproductive health services. Genet Mengistu, the Executive Director of the Family Guidance Association of Ethiopia (FGAE), an IPPF member, said: "This is an incredible opportunity to accelerate change for women and girls to decide their own futures. It will get family planning services to Ethiopian women, particularly to those underserved." Simon Cooke, CEO at MSI, said: "Through this funding, we and our partners will be able to bring quality sexual and reproductive health services to millions of women in some of the world’s poorest and most marginalised communities. For many, it will be their first chance to access any kind of contraception, empowering them to stay in education, forge a career, stay healthy and pursue their hopes and dreams for the future. With this landmark investment in women and girls, the UK Government is creating the right conditions to drive multiple other areas of development, from increasing the number of girls completing education to enabling couples and families in poverty to maximise their earning potential. We applaud DFID for its continued support for this vital and life-changing work." The £200 million investment to leading sexual and reproductive health service providers IPPF and MSI is made-up of two individual DFID WISH awards, through consortium arrangements. Lot 1 is a consortium managed by MSI with 7 of its country programmes and 6 IPPF Member Associations, with a focus on West and Central Africa. Lot 2 is a consortium managed by IPPF with 16 Member Associations and 8 MSI country programmes with a focus on East and Southern Africa and Asia.
IPPF welcomes UNFPA's State of the World Population 2018 report
The UNFPA's State of the World Population report highlights that, while much progress has been made globally in upholding reproductive rights, there remains large inequalities in access and high levels of unmet needs. By grouping countries into low, medium and high fertility countries, the report recognizes the diverse needs globally, and the importance of targeted interventions. In high fertility countries, the high unmet need for family planning is one of the most important issues that governments and SRHR partners need to address by ensuring access to quality, rights-based contraceptive services. In low fertility countries, the report highlights infertility and needs of the ageing population - more needs to be done to prioritize these issues, especially in countries with low fertility. In countries with mid fertility, high adolescent fertility is a concern, and reflects the need to further strengthen youth friendly services, including comprehensive sexuality education. IPPF supports the report and especially its emphasis and recognition of the reproductive rights of couples, including the right to choose, the right to decide the number of children they wish to have and when, throughout the report. IPPF joins its voice with UNFPA and partners to call on governments to sustain their commitments to SRHR and ensure access to the full range of high quality universally accessible SRH services and allocate domestic funding to ensure that gender equality and sexual and reproductive rights are realized. This is of critical importance as the 25th anniversary of the historic commitments adopted by 179 governments in the Programme of Action of the International Conference of Population and Development in Cairo in 1994. IPPF aligns with the call made by the report on the rights of all women to choose and decide freely and without question over their bodies, sexuality and reproduction as a priority to achieve the agenda 2030.
World Contraception Day: Contraceptive funding in crisis
On this World Contraception Day, some 214 million women and girls in developing regions have an unmet need for modern contraception. These are women and girls who want to avoid a pregnancy but are not using a modern method of contraception. While the reasons for this are multiple, the costs and availability of contraception remain major barriers. Access to contraception is a basic human right. Governments affirmed women’s right to have access to safe, effective and affordable methods of contraception of their choice 24 years ago, at the International Conference on Population and Development in Cairo. In 2015, in the landmark Sustainable Development Goals, governments pledged to ensure universal access to family planning by 2030. Yet, three years on, global funding for contraceptives is in crisis. There is a major gap between needs for funding for contraceptives and the resources provided by both domestic and donor governments. In low- and middle-income countries out-of-pocket payments by individuals account for more than 80% of all spending on contraceptives. Domestic governments only provide around 8% of spending, while donors fund 10%. Out-of-pocket spending is an inequitable form of financing health services. Those least able to afford it carry most of the cost burden. The impact on household finances exacerbates inequalities and pushes people further into poverty. The gender implication is huge. Women and girls rely heavily on access to contraceptives and reproductive healthcare, and yet many do not have the financial means. Demand for contraceptives is expected to increase, which will further widen existing funding gaps. Estimates of the difference between today’s spending on contraceptives and the cost of meeting projected needs in low- and middle-income countries in 2020 show an additional funding gap of US$290m if current trends in use continue. Unless domestic or donor government finance increases substantially, most of this gap will have to be met by relying on user fees. Domestic governments have the main responsibility for ensuring access to contraception, yet donors continue to play an important role, particularly in the world’s poorest countries. In the 31 lowest income countries, donors currently finance 65% of all contraceptives, while domestic governments fund 7%. Individuals’ out-of-pocket spending accounts for 28%. Yet, while donor funding remains essential, it has faced a downward trend in recent years. Funding from the United States, the largest family planning donor, has been fairly stable but is now at risk. Funding pledges made by European and other donors in 2017 in support of the She Decides initiative and at the July London Family Planning Summit are promising, but it is too soon to tell whether they will bring a reversal in longer term funding trends. Domestic governments must live up to their responsibility to increase their funding and ensure access to contraception and healthcare. Yet, donors must also continue and step up their support. Millions of women and girls depend on it. - Raffaela Dattler, Financing for Development Advisor, IPPF
Integration of DMPA‑SC into the method mix contributes to increased uptake of all methods of family planning
Injectable contraceptives are an increasingly popular method of family planning. They are safe, discrete, highly effective, and generally last for several months. Sayana® Press, also known as subcutaneous depot medroxyprogesterone (DMPA‑SC), is a lower‑dose formula version of the already popular injectable Depo‑Provera. DMPA‑SC combines the drug and needle in a single‑use unit, which makes it easy to transport and simple to use with little training. DMPA‑SC can be administered by community health workers (CHWs) and women themselves – potentially making injectable contraceptives available to women who can’t easily travel to clinics.
IMAP Statement on emergency contraception
Emergency contraception (EC) refers to any contraceptive method that can be used after having unprotected or inadequately protected sexual intercourse (UPSI) but before pregnancy occurs, providing women with the opportunity to prevent an unwanted pregnancy. EC is a safe and effective method for preventing unwanted pregnancy and can reduce the risk of pregnancy by up to 99%. In spite of its effectiveness, EC is not frequently used. In many countries, women face barriers to accessing EC. The majority of women in low‑income countries are unaware of EC. Moreover, some providers have negative attitudes toward providing EC to women and girls.

Myth-busting facts about the contraceptive injection
Watch this short animation to learn more about the contraceptive injection, a contraceptive method that requires no daily action and doesn't interfere with sex. Learn more about other methods
Pagination
- Previous page
- Page 7
- Next page






